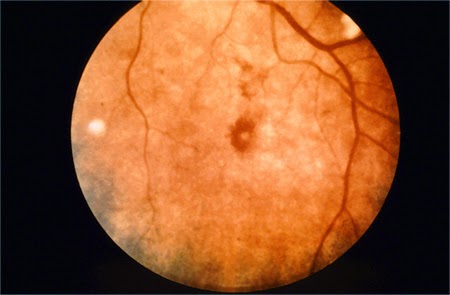
A 17 year old girl was admitted in the hospital with a 6 month history of generalized body pains, loss of weight and night sweats. Over the past 6 weeks she has started to become breathless on mild exertion. At the time of admission she had a temperature of 101 F and on examination she had a early diastolic murmur on the left sternal border on auscultation of the precordium. On doing a fundoscopic examination following was seen:
Roth spots in the retina ( hemorrhagic area with a pale center)
On examination of her hands subungal splinter hemorrhage was seen in one of the finger nails. The picture is shown below:
What is the most likely diagnosis?
Study and Memorize Medical Conditions With The Help Of Photos. Useful Site For Medical Students, Doctors And Nurses.
Thursday, April 30, 2015
A 12 Year Old Girl Presents With Abdominal Pain, Bloody Diarrhea And A Purpuric Rash.
A 12 year old girl is admitted to the pediatric ward with a 2 day history of Lower abdominal pain and blood stained diarrhea. Three days later she began to complain of pain in her ankles and the right elbow. She also felt nauseous but there was no history of vomiting.
On examination the patient looks sick, has a periorbital edema and a purpuric rash affecting the arms and the legs.
The picture of her rash on lower extremeness is shown below:
She is afebrile but her BP is 150/95 mmHg.
The lab workup and the results are given below:
On examination the patient looks sick, has a periorbital edema and a purpuric rash affecting the arms and the legs.
The picture of her rash on lower extremeness is shown below:
She is afebrile but her BP is 150/95 mmHg.
The lab workup and the results are given below:
- Hb = 10g/dl
- WBC= 12000/cmm
- Platelets= 135,000/cmm
- ESR= 35
- PT = 13 sec (control= 13 sec)
- aPTT= 34 sec ( control= 36 sec)
- Sodium=138 mmol/l
- Potassium= 5.9mmol/l
- Urinalysis= Blood++, Protein++
Based on the above history and investigations what is the most probable diagnosis?
?
?
?
.
Henoch-Schonlein Purpura ( The combination of lower abdominal pain, bloody diarrhea, purpuric rash, nephritis, and a high blood pressure in a young girls are all suggestive of the disease)
Tuesday, April 28, 2015
A 40 Year Old Woman Presents With Sudden Facial Asymmetry
A 40 year old woman woke up in the morning and felt her left side of the face being peculiar and heavy. On looking in the mirror she saw that the corner of her mouth on the left side was drooping and her left lower eyelid seemed to be lower than her right. When she attempted to smile her left side of the face remained immobile and broad like. On eating her breakfast she felt the food to stick on the left side of her cheek. She was terrified and came to the emergency department for a checkup.
On examination she has paralysis of the entire left side of her face.
The picture of the lady is shown below:
Diagnosis: Bell's Palsy ( Caused by a lesion of the left facial nerve that supply the muscles of facial expression).
Case Discussion:
Bell's palsy is a paralysis or weakness of one side of the face caused by a damage to the facial nerve. The condition comes on suddenly usually overnight and fortunately gets better on its own over a few weeks.
On examination she has paralysis of the entire left side of her face.
The picture of the lady is shown below:
Diagnosis: Bell's Palsy ( Caused by a lesion of the left facial nerve that supply the muscles of facial expression).
Case Discussion:
Bell's palsy is a paralysis or weakness of one side of the face caused by a damage to the facial nerve. The condition comes on suddenly usually overnight and fortunately gets better on its own over a few weeks.
Monday, April 27, 2015
A 38Year Old Man Presents With A Six Week History Of Dyspnoea and Wheezing
A 38 year old man presents with history of difficulty breathing and wheezing that has started about six weeks back, For 2 weeks he has also developed cough productive of yellow sputum and fever. There is no history of night sweats.
The patient has a past history of asthma and recurrent atopic symptoms.
A Chest X ray done as a part of diagnostic workup is shown below:
X ray findings show diffuse peri-hilar infiltrates.
On blood workup there was an eosinophillia and the sputum culture was negative.
Based on the above history and investigations for is the most likely diagnosis?
Allergic bronchopulmonary aspergillosis
Case Discussion:
The patient has a past history of asthma and recurrent atopic symptoms.
A Chest X ray done as a part of diagnostic workup is shown below:
X ray findings show diffuse peri-hilar infiltrates.
On blood workup there was an eosinophillia and the sputum culture was negative.
Based on the above history and investigations for is the most likely diagnosis?
Allergic bronchopulmonary aspergillosis
Case Discussion:
A 68 year Old Woman With Rheumatoid Arthritis Presents With Swollen Ankles
A 68 year old woman who was diagnosed with rheumatoid arthritis about 20 years ago now presents with swollen ankles and edematous feet. Her rheumatoid arthritis was relatively well controlled with non steroidal anti inflammatory drugs until six months ago when her symptoms of pain and swelling needed the addition of penicillamine. Patient also has a history of hypertension controlled with drugs.
On examination she has symmetric joint deformities consistent with long standing rheumatoid arthritis. The picture of her hands is shown below:
Her heart rate was 90 beats/min and irregular. Her blood pressure was 140/90 mm Hg. JVP was not raised and her heart sounds were normal and chest was clear on auscultation.
Inspection of the lower limbs reveal pitting edema. Picture is shown below:
On investigation urinalysis shows +++ proteinuria.
What is the cause of her edema and what will be the management??
On examination she has symmetric joint deformities consistent with long standing rheumatoid arthritis. The picture of her hands is shown below:
Her heart rate was 90 beats/min and irregular. Her blood pressure was 140/90 mm Hg. JVP was not raised and her heart sounds were normal and chest was clear on auscultation.
Inspection of the lower limbs reveal pitting edema. Picture is shown below:
On investigation urinalysis shows +++ proteinuria.
What is the cause of her edema and what will be the management??
Sunday, April 26, 2015
A 20 Year Old College Student Complains Of Chest Pain And Shortness Of Breath During Exercise
A 20 year old college student comes to his physician concerned about his health because he feels chest pain and gets short of breath during exercise or sports. He also describes having episodes of feeling his heart beat very fast. He wanted to have workup done because his brother died suddenly at an age of 18 years while participating in his school sports event.
On examination the patient is a healthy looking young man and there were no abnormalities detected on his chest examination.
An ECG was done which is shown below:
The above ECG is notable for inverted T waves, and deep narrow dagger like Q waves in the leads V4, V5 and V6
On Echocardiography there is septal hypertrophy with left ventricular outflow tract obstruction.
Based on the ECG and the history of the patient what is the most probable diagnosis?
.
.
Hypertrophic Obsstructive cardiomyopathy
On examination the patient is a healthy looking young man and there were no abnormalities detected on his chest examination.
An ECG was done which is shown below:
The above ECG is notable for inverted T waves, and deep narrow dagger like Q waves in the leads V4, V5 and V6
On Echocardiography there is septal hypertrophy with left ventricular outflow tract obstruction.
Based on the ECG and the history of the patient what is the most probable diagnosis?
.
.
Hypertrophic Obsstructive cardiomyopathy
Friday, April 24, 2015
A 16 Year Old Girl With A Past History Of Chemotherapy Presents With Breathlessness.
A 16 year old girl who had a past history of acute myeloid leukemia and was treated with six courses of chemotherapy presents to her doctor with the complain of Breathlessness on exertion. During her chemotherapy she was also given cyclophosphamide. On examination patient appears to be breathless even at rest and she looks cyanosed. There is no evidence of clubbing. Her lung function test shows FEV1/FVC ratio of 80%, but there is a decreased total lung capacity, indicating a restrictive pattern.
Her chest X ray is shown below:
The X ray shows diffuse infiltrates indicative of interstitial lung disease.
What is the cause of patient's symptoms in the above mentioned case?
Answer: Cyclophosphamide induced lung fibrosis.
Case Discussion:
Cyclophosphamide induced lung fibrosis is a relatively rare condition and is most likely to occur in patients who had concomitant pulmonary radiation or has taken other drugs that are toxic to the lungs. Patients may present several years after the cessation of treatment and with advanced damage to the lungs.
The diagnosis is usually clinical from the history of exposure to the drug and from restrictive lung defect on pulmonary function test. The chest X ray shows reticulonodular shadowing more so in the upper zones.
Her chest X ray is shown below:
The X ray shows diffuse infiltrates indicative of interstitial lung disease.
What is the cause of patient's symptoms in the above mentioned case?
Answer: Cyclophosphamide induced lung fibrosis.
Case Discussion:
Cyclophosphamide induced lung fibrosis is a relatively rare condition and is most likely to occur in patients who had concomitant pulmonary radiation or has taken other drugs that are toxic to the lungs. Patients may present several years after the cessation of treatment and with advanced damage to the lungs.
The diagnosis is usually clinical from the history of exposure to the drug and from restrictive lung defect on pulmonary function test. The chest X ray shows reticulonodular shadowing more so in the upper zones.
A 53 Year Old Man With A Long History Of Asthma Presents With Blood In Urine
A 53 year old man with a history of asthma and allergic rhinitis was admitted to the hospital with acute breathlessness, cough and presence of blood in urine. On examination , he appears pale and unwell. His pulse is 90 beats/ minute and Blood pressure 160/90 mm Hg. Abdominal and chest examination did not reveal any significant abnormalities. Urinalysis shows ++ for blood and protein. Complete blood count shows Hb = 7 g/dl, WBC = 11000/dl with a high percentage of eosinophils, increased ESR and slightly raised urea and creatinine. A biopsy was taken and shows the following histologic picture:
An eosinophillic vasculitis
What is the diagnosis?
.
.
Churg- Strauss Syndrome
Case Discussion:
Churg- Strauss Syndrome which is also known as Eosinophillic granulomatosis is a rare autoimmune condition that affects small and medium sized arteries and veins.
American College of Rheumatology proposed the following six criteria for the diagnosis of Churg- Strauss Syndrome.
An eosinophillic vasculitis
What is the diagnosis?
.
.
Churg- Strauss Syndrome
Case Discussion:
Churg- Strauss Syndrome which is also known as Eosinophillic granulomatosis is a rare autoimmune condition that affects small and medium sized arteries and veins.
American College of Rheumatology proposed the following six criteria for the diagnosis of Churg- Strauss Syndrome.
Thursday, April 23, 2015
A 65 Year Old Diabetic Man Has a Ulcer With A Draining Sinus Tract On His Leg
A 65 year old man with known case of diabetes and peripheral vascular disease complains of pain in his leg where he has an old ulcer with a draining sinus tract. Along with other investigations an X ray was done which is shown below:
Central part showing an ill defined osteolytic area and major part consists of reactive sclerosis.
The patient was diagnosed to have Osteomyelitis.
Case Discussion.
Osteomyelitis in adults almost always presents in patients with underlying diabetes, peripheral vascular disease or both with an ulcer or a soft tissue infection.
Clinical features: May include:
Central part showing an ill defined osteolytic area and major part consists of reactive sclerosis.
The patient was diagnosed to have Osteomyelitis.
Case Discussion.
Osteomyelitis in adults almost always presents in patients with underlying diabetes, peripheral vascular disease or both with an ulcer or a soft tissue infection.
Clinical features: May include:
- Fever
- Irritability in case of children
- Pain, swelling and warmth in the area of infection.
Causes: Most cases of osteomyelitis are cause by the bacterial Staphylococcus aureus. It can spread to involve the bone via the blood stream, through a nearby infection of the skin or by direct contamination
Complications: include:
40 Year Old Man With Prominent Supra Orbital Ridges And A Large Lower Jaw
On examination the patient appears to be a tall man with prominent supra orbital ridges, ans a large lower jaw. His hands and feet appear to be large and his skin seems to be thickened and greasy.
The patients picture taken in the doctor's office is shown below:
What is the diagnosis?
Acromegaly.
What other endocrine disorders a patient with acromegaly may have?
7 Year Old Male Child Presents With Pallor and Dark Urine While On Treatment For Malaria
A 7 Year old child who presented with high grade fever about 5 days back and is now on treatment for malaria now presents to the emergency with severe, sudden onset of pallor and dark colored urine. He feels very weak and is frightened by the appearance of his urine. Although he is afebrile now, he is breathing rapidly and on examination he looks pale and there is yellowish discoloration of his skin and sclera. On abdominal examination, spleen is enlarged and palpable.
Labwork shows:
Hb = 5 gm/dl
Increased reticulocyte count
Increased billirubin levels.
The peripheral blood film has the following picture:
Numerous destroyed red blood cells ( Arrows shows bite cells following removal of Heinz bodies).
What is the Diagnosis?
.
.
.
Hemolytic anemia due to G6PD deficiency, in this case hemolysis triggered due to antimalarial drugs.
Labwork shows:
Hb = 5 gm/dl
Increased reticulocyte count
Increased billirubin levels.
The peripheral blood film has the following picture:
Numerous destroyed red blood cells ( Arrows shows bite cells following removal of Heinz bodies).
What is the Diagnosis?
.
.
.
Hemolytic anemia due to G6PD deficiency, in this case hemolysis triggered due to antimalarial drugs.
Wednesday, April 22, 2015
A 27 Year Old Woman Complains Of Dysuria And Suprapubic Pain
A 27 year old woman presents to her primary care physician with the complains of increased urinary frequency, pain and burning on urination as well as pain in the supra pubic area for the last 2 days. She also noticed that she had fever last night. She took acetaminophen which gave her temporary relief. Patient remembers having similar symptoms a few months back. She is sexually active with her husband. Her menstrual cycle is normal and regular.
On Examination patient is febrile with a temperature of 101 F. On abdominal examination she feels discomfort on palpation in the supra pubic region.
She is advised to get some lab workup done including a urine dipstick which revealed +ve nitrites and + leukocytes. Her urine is sent for culture which showed the following picture in the lab.
Culture in the laboratory showing growth of Escherichia Coli.
Patient is diagnosed as a case of Urinary tract infection.
Case Discussion:
On Examination patient is febrile with a temperature of 101 F. On abdominal examination she feels discomfort on palpation in the supra pubic region.
She is advised to get some lab workup done including a urine dipstick which revealed +ve nitrites and + leukocytes. Her urine is sent for culture which showed the following picture in the lab.
Culture in the laboratory showing growth of Escherichia Coli.
Patient is diagnosed as a case of Urinary tract infection.
Case Discussion:
Tuesday, April 21, 2015
A 25 Year Old Man Complains Of Occasional Blood In Stool
A 25 year old man comes to his primary care physician and complains of seeing blood in his stool occasionally. He has fairly regular and normal bowel habits but he is concerned because he has lost his father at a young age due to colon cancer and his initial symptoms were also blood in stool. He has no other symptoms and is living a healthy life style.
The patient was referred for a colonoscopy which showed the following in the sigmoid colon.
Multiple polyps carpeting the mucosa of the colon.
Based on the history and the above picture what is the most probable diagnosis?
.
.
.
Familial adenomatous polyposis
Case Discussion:
The patient was referred for a colonoscopy which showed the following in the sigmoid colon.
Multiple polyps carpeting the mucosa of the colon.
Based on the history and the above picture what is the most probable diagnosis?
.
.
.
Familial adenomatous polyposis
Case Discussion:
A 43 Year Old Hospitalized Man Complains Of Sudden Episodes Of Dizziness and Lightheadedness
A 43 year old man who is hospitalized with Symptoms of heart failure complains of sudden episodes of dizziness and lightheadedness, he was otherwise fine and was responding to the treatment for heart failure. An ECG was done and shows the following appearance:
What is the diagnosis on the basis of characteristic appearance on the ECG.
?
?
?
Atrial Flutter ( Saw tooth waves on ECG )
Case Discussion:
Atrial Flutter is an abnormal heart rhythm and is one of the types of supraventricular tachycardia. It is similar to atrial fibrillation and sometimes both may occur one after the other.
Risk Factors: Certain underlying medical conditions increase the risk of developing atrial flutter, theses may include:
What is the diagnosis on the basis of characteristic appearance on the ECG.
?
?
?
Atrial Flutter ( Saw tooth waves on ECG )
Case Discussion:
Atrial Flutter is an abnormal heart rhythm and is one of the types of supraventricular tachycardia. It is similar to atrial fibrillation and sometimes both may occur one after the other.
Risk Factors: Certain underlying medical conditions increase the risk of developing atrial flutter, theses may include:
- Heart failure
- Previous heart attack
- Valvular abnormalities
- High blood pressure
- Recent surgery
- Thyroid disorders
- Diabetes
- Alcoholism
- Chronic lung disease
Monday, April 20, 2015
A 30 Year Old Man Presents With A Bloody Diarrhea, Fever and Abdominal Pain
A 30 year old man presents to his primary care physician with the complains of severe abdominal pain, high grade fever and a bloody diarrhea that started 2 days ago. Initially the symptoms were mild but now he is feeling very sick and weak. He gives a history of passing more than 5 watery stools mixed with blood today. He has no history of vomiting but his appetite has decreased. He remembers eating at a road side restaurant while he was coming home from work. On examination he looks pale and mildly dehydrated.
Hos fresh stool specimen is collected and examined under the microscope which shows the following picture:
The above picture shows the shigella species under microscope in a stool specimen.
The patient was diagnosed as a case of Bacillary dysentery or Shigellosis
Hos fresh stool specimen is collected and examined under the microscope which shows the following picture:
The above picture shows the shigella species under microscope in a stool specimen.
The patient was diagnosed as a case of Bacillary dysentery or Shigellosis
A 50 Year Old Man Who Has Been Chronically Sick Presents With Weight Loss, Cough And Weakness
A 50 year old man who has been sick for the past 5 years with fever, cough and fatigue and has been taking incomplete treatments from different primary care physicians presents with a cough, fever, weight loss, night sweats, extreme body weakness and pain through out the body. He was taking some cough syrups recently with no improvement in his symptoms.
On Examination patient is a thin man with poor hygiene and signs of weight loss. He is anemic and has palpable lymph nodes in his neck and axilla. He is coughing most of the time during the examination. He has decreased breath sounds through out the lung filed and on abdominal examination the spleen is enlarged.
His Chest X ray is shown below:
Based on the above history and the X ray picture what is the most probable diagnosis?
.
.
Miliary Tuberculosis.
Case Discussion:
Miliary Tuberculosis is an uncommon manifestation of pulmonary tuberculosis and it represents hematogenous dissemination of uncontrolled tuberculous infection.
On Examination patient is a thin man with poor hygiene and signs of weight loss. He is anemic and has palpable lymph nodes in his neck and axilla. He is coughing most of the time during the examination. He has decreased breath sounds through out the lung filed and on abdominal examination the spleen is enlarged.
His Chest X ray is shown below:
Based on the above history and the X ray picture what is the most probable diagnosis?
.
.
Miliary Tuberculosis.
Case Discussion:
Miliary Tuberculosis is an uncommon manifestation of pulmonary tuberculosis and it represents hematogenous dissemination of uncontrolled tuberculous infection.
A 60 Year Old Man With Fever, Productive cough and Weight Loss
A 60 year old man is referred to a pulmonary specialist with the complains of high grade fever with chills, a productive cough for about 4 weeks and a history of weight loss. The patient complains of a purulent sputum which is sometime streaked with blood and about a tablespoon full in quantity. His wife says that she has noticed a foul smell from his breath.
Patient has brought the following X ray with him that was done a day before:
Chest x-ray demonstrates a large intrapulmonary cavity with an irregular air/fluid level interiorly. The wall of the cavity is ill-defined, ranging from very thin and smooth laterally to somewhat nodular superomedially.
The Patient is diagnosed as a case of Lung Abscess
Case Discussion:
Lung Abscess:
Lung abscess is defined as a cavitating area of localized , suppurative infection within the lung.
Causes: A lung abscess may occur due to :
Patient has brought the following X ray with him that was done a day before:
Chest x-ray demonstrates a large intrapulmonary cavity with an irregular air/fluid level interiorly. The wall of the cavity is ill-defined, ranging from very thin and smooth laterally to somewhat nodular superomedially.
The Patient is diagnosed as a case of Lung Abscess
Case Discussion:
Lung Abscess:
Lung abscess is defined as a cavitating area of localized , suppurative infection within the lung.
Causes: A lung abscess may occur due to :
A 35 Year Old Man Goes For Physical Examination For Job Fitness
A 35 year old man is having a physical examination as a requirement for job fitness. He is asked to do a pulmonary function test and blow through a spirometer.
What is spirometry?
Spirometry is a powerful tool that helps measure the functional lung volumes and detect any underlying obstructive or restrictive lung disorders.
Below is a graph to help understand lung volumes:
What is spirometry?
Spirometry is a powerful tool that helps measure the functional lung volumes and detect any underlying obstructive or restrictive lung disorders.
Below is a graph to help understand lung volumes:
Spirometric values
|
Friday, April 17, 2015
A 5 Year Old African Child With Swelling Of The Jaw
A 5 year old African child is referred to a Pediatrician for the presenting symptoms of a progressive painless swelling of the jaw that has not responded to antibiotic treatment and is growing rapidly leading to disfiguring of the face. The child has low grade fever for over 4 months and has also lost weight. He has lost his appetite and interest in daily activities.
The picture is shown below:
Blood workup shows Anemia and low platelet count. Serum LDH was markedly elevated and serum uric acid levels were also high.
A biopsy was taken from the tumor and the case was diagnosed as Burkitt Lymphoma.
Case Discussion:
BURKITT LYMPHOMA
Burkitt lymphoma is a form of non Hodgkin's lymphoma in which the cancer cells start in the immune cells known as B cells.
The picture is shown below:
Blood workup shows Anemia and low platelet count. Serum LDH was markedly elevated and serum uric acid levels were also high.
A biopsy was taken from the tumor and the case was diagnosed as Burkitt Lymphoma.
Case Discussion:
BURKITT LYMPHOMA
Burkitt lymphoma is a form of non Hodgkin's lymphoma in which the cancer cells start in the immune cells known as B cells.
Thursday, April 16, 2015
A 3 Year Old Boy With Sudden Choking While Playing With His Toys
A 3 year old boy is brought to the emergency department when he was seen to have a sudden choking while he was normal and playing with his toys. He has no history of any respiratory infection.
The Chest X ray is shown below:
What is the most probable diagnosis?
Inhaled foreign body
Case Discussion:
The Chest X ray is shown below:
What is the most probable diagnosis?
Inhaled foreign body
Case Discussion:
A 45 Year Old Man Presents With Abdominal Distention
A 45 year old man is brought to the doctor's office by his wife in a confused state, and complains of fatigue, weakness and pain under his right rib cage for the past several months. He is a drug abuser and has a history of jaundice in the past. His wife says he has been diagnosed with hepatitis C but they don't have any medical record with them.
On examination the patient is acting strangely and is not able to give a proper history. He has anemia and a mild jaundice. His abdomen is distended, tender and firm with prominent veins at the umbilicus. Liver and spleen are both enlarged and palpable.
The lab work shows:
On examination the patient is acting strangely and is not able to give a proper history. He has anemia and a mild jaundice. His abdomen is distended, tender and firm with prominent veins at the umbilicus. Liver and spleen are both enlarged and palpable.
The lab work shows:
- AST = 145 IU/L
- ALT = 150 IU/L
- Serum total billirubin = 7.5 mg/dl
- PT = 18.2
The patient's bedside abdominal view is shown below:
Based on the given history in the above case what is the most likely case of the patient's abdominal distension?
Wednesday, April 1, 2015
A 50 Year Old Man Presents With Fatigue And Easy Bruising
A 50 year old man presents to his primary care physician with complains of fatigue and recently noticed having bruises after minor trauma. Although he has never taken his temperature he feels that he has low grade fever on and off over the last few months.
On Examination he was noticed to have an enlarged spleen and few bruises.
His blood workup showed low RBC, WBC and platelet count. The peripheral smear is shown below:
What is the Diagnosis?
.
.
.
Hairy cell leukemia
On Examination he was noticed to have an enlarged spleen and few bruises.
His blood workup showed low RBC, WBC and platelet count. The peripheral smear is shown below:
What is the Diagnosis?
.
.
.
Hairy cell leukemia
Subscribe to:
Posts (Atom)